99.5% accuracy · ISO 27001 certified
Insurance Claims Data Entry Services
Claims backlogs cost you money and customer trust. Acelerar’s trained insurance data specialists process claims accurately and on time - extracting data from forms, verifying details, and entering records into your claims management system.




















Insurance Claims Processing
What is insurance claims data entry?
Insurance claims data entry is the process of extracting, verifying, and entering information from insurance claim forms into claims management systems and databases. This includes policyholder details, claim amounts, incident descriptions, supporting document data, and adjuster notes. For insurance companies, TPAs, and claims processing firms, the speed and accuracy of claims data entry directly impacts settlement timelines, customer satisfaction, and regulatory compliance. Outsourcing claims data entry gives you trained specialists who process claims accurately, reduce denial rates, and clear backlogs faster.
Market Data
The data entry outsourcing market
Businesses worldwide are outsourcing data entry to reduce costs and improve accuracy.
What We Handle
End-to-end claims data processing
Claims data extraction & entry
We extract data from paper claim forms, scanned documents, emails, and faxes, then enter it into your claims management system. Policyholder info, claim numbers, dates of loss, coverage details, and claim amounts - every field verified for accuracy before submission.
See form processing services →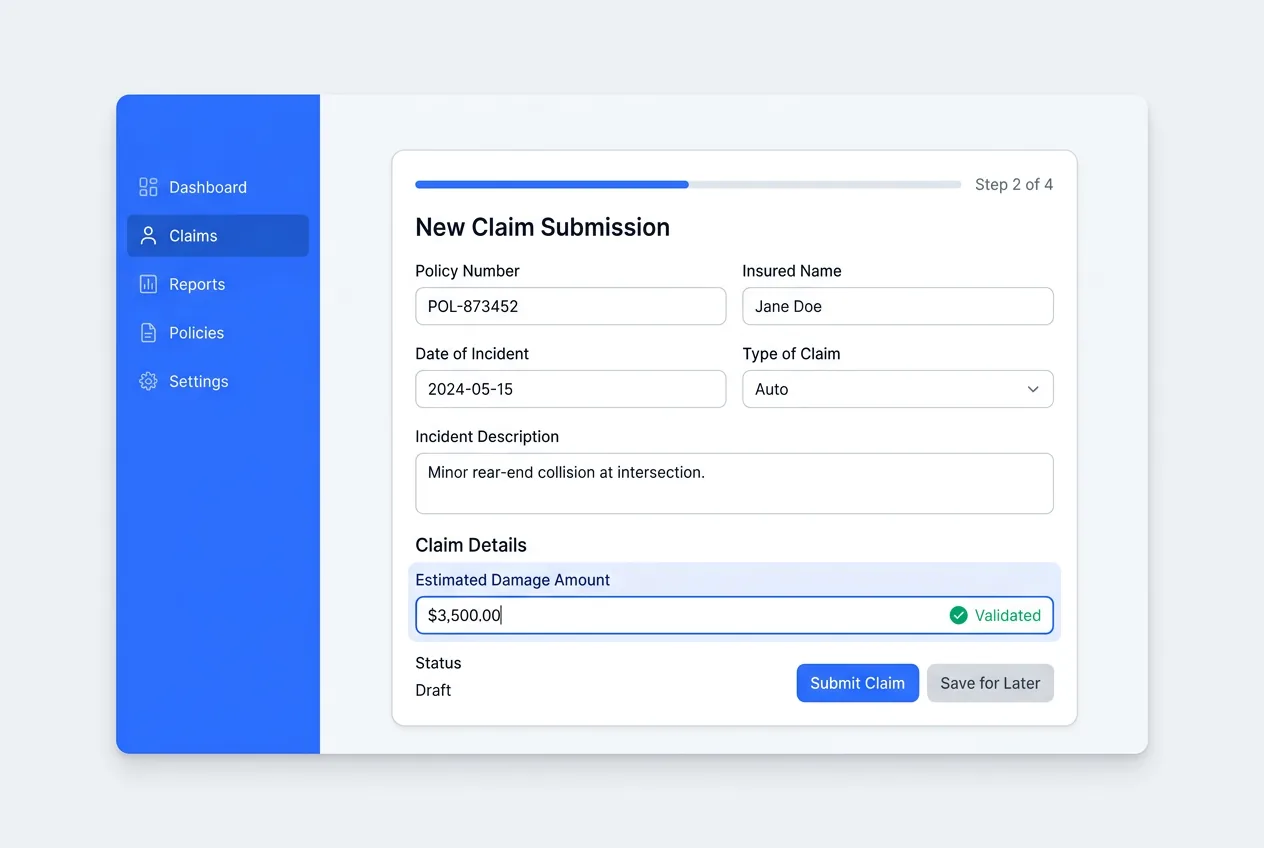
Claims verification & reconciliation
Our teams cross-reference claim data against policy records, verify coverage eligibility, flag discrepancies, and reconcile supporting documentation. Reduce first-pass denial rates with accurate, complete claim submissions.
See data processing services →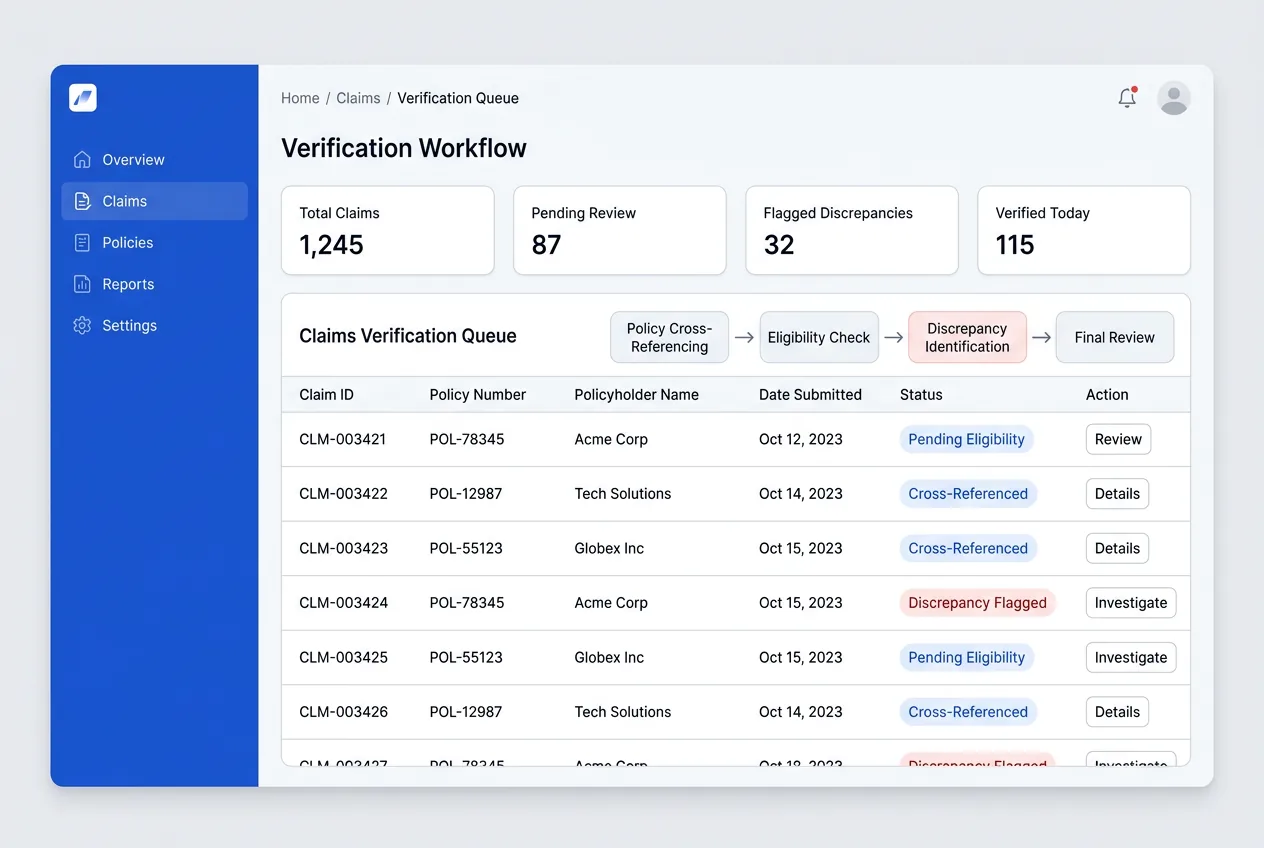
Cost Comparison
In-house claims data entry vs. Acelerar
$48K/yr
per year / per person
Salary, benefits, training, compliance certifications, and management overhead for one full-time US-based claims processor
$15K/yr
per year / per person
Fully loaded rate includes salary, infrastructure, AI tools, QA, and dedicated account manager
Why Outsource Claims Processing
Why insurance companies outsource claims data entry to Acelerar
99.5% First-Pass Accuracy
Inaccurate claims data leads to denials, delays, and rework. Our double-key verification catches errors before they become costly rejections.
Same-Day Processing
Standard claims are processed same-day. High-volume batches (1,000+ claims) are scoped with custom SLAs. Rush processing available for priority claims.
ISO 27001 Certified Security
Insurance data is sensitive. Our ISO 27001 certified operations, NDA coverage, and encrypted transfers protect policyholder information at every touchpoint.
70% Cost Reduction
A claims processor in the US costs $35,000-$45,000/year. Our dedicated teams process the same volume at 70% less cost with higher accuracy.
How It Works
From claim forms to processed records in 4 steps
Receive
Send claims in any format: paper scans, PDFs, emails, faxes, or digital submissions.
Extract
Our team extracts all relevant data from claim documents with field-level verification.
Verify
Claims data is cross-referenced against policy records and flagged for discrepancies.
Enter
Verified claim records are entered into your claims management system, ready for adjudication.
Claims backlog slowing you down?
Tell us your claims volume and current backlog. We’ll have a processing plan ready within 24 hours.
Get a Free QuoteWe work with your tools
Our teams are trained on the platforms you already use.
What our data entry clients say
“The Acelerar team is a self-sustaining machine. They’ve become an extension of our own team.”
“Acelerar handled our entire catalog migration (50,000+ SKUs) without a single missed deadline.”
“We needed reliable, fast data entry at scale. Acelerar delivered consistent quality from day one, no ramp-up time needed.”
Industry Outlook
Where data entry outsourcing is heading
The outsourcing industry is growing, and AI is reshaping how data operations are delivered.